
Quick Quality Healthcare
Journey To Excellence
Clinical Governance
A Structured Effort That Transforms Care

Clinical governance is the system through which healthcare organizations are accountable for continuously improving the quality of care and safeguarding high standards. It creates an environment where excellence in clinical practice can thrive and ensures that services are safe, effective, patient-centered, and evidence-based.
While corporate governance focuses on the overall direction and accountability of the organization, clinical governance operates at the frontlines—guiding patient care decisions, professional practice, and service delivery. In many hospitals, it is overseen by a Clinical Governance Committee, typically chaired by a senior clinician and supported by a multidisciplinary team. This body reports to both hospital leadership and the board to align clinical and organizational goals.
Originating in the UK as a response to clinical failures, clinical governance is implemented through an organized system of structures, processes, leadership, and culture that collectively ensure accountability for the safety and quality of clinical care.
Benefits of a Strong Clinical Governance System
Improves patient safety and clinical outcomes
Ensures accountability for clinical performance
Builds staff confidence, morale, and professionalism
Strengthens compliance with accreditation and regulatory requirements
Enhances transparency and public trust in healthcare services
What Happens Without Strong Clinical Governance?
Inconsistent care standards → Increased variability in outcomes and risk of patient harm.
Undetected safety risks → Delays in identifying preventable incidents or system failures.
Professional complacency → Lack of accountability for clinical performance or ongoing development.
Misalignment with organizational goals → Quality improvement remains fragmented and disconnected from strategic priorities.
Regulatory non-compliance → Risk of losing accreditation, reputation damage, or legal consequences.
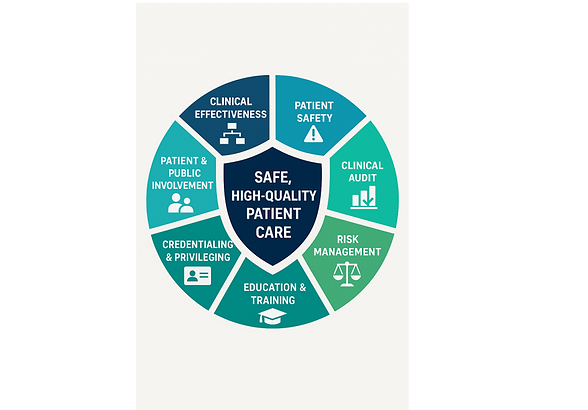
Key Components of Clinical Governance:
Patient Safety: Systems to identify, report, and reduce risks, errors, and adverse events.
Clinical Effectiveness: Promoting evidence-based care and outcomes monitoring. Uphold best practices across specialties.
Clinical Risk Management: Identifying clinical risks and mitigating them through proactive systems.
4. Audit and Performance Monitoring: Regular clinical audits and review of outcomes to improve care. Tracks indicators such as infection rates, readmission rates, surgical outcomes, and mortality data to ensure quality benchmarks are met.
5. Foster professional development and credentialling: Ongoing education and training to maintain competency.
6. Patient, family and Public Involvement: Ensuring care is responsive to patient needs, preferences, and experiences by appropriate response to complaints , feedback systems and service design.
7. Staff Management and Engagement: Supporting a culture of accountability, teamwork, and leadership in clinical teams.
8. Uphold Clinical Ethics and Standards: Guides ethical clinical decision-making, patient autonomy, confidentiality, and professional conduct across all disciplines.
9. Ensure Compliance with Clinical Regulations and Accreditation: Aligns clinical practices with national standards, licensing requirements, and external accreditation bodies.
Establishing a Clinical Governance Framework in a Hospital
Governance that protects patients, empowers staff, and drives excellence.”
1. Secure Leadership Commitment
Start with the CEO and executive leadership team. Clinical governance must be seen as a shared responsibility between management and clinicians.
Appoint a clinical governance lead—often a senior clinician or medical director—responsible for building and overseeing the program.
2. Form a Clinical Governance Committee
Define clear terms of reference, reporting lines (to the CEO and/or Board), and meeting schedules.
Create clinical Governance Committee, a multidisciplinary group which typically includes department and committee heads, doctors, nurses, allied health professionals, quality officers, and possibly board representatives.
Define clear roles and responsibilities for clinical governance at all levels—board, executive team, department heads, and frontline staff.
Integrate with Hospital Strategy and Operations
Align clinical governance with hospital goals, strategic planning, risk management, and quality improvement initiatives.
Use data (e.g., clinical indicators, safety events, patient feedback) to inform decisions and monitor performance.
3. Develop a Clinical Governance Framework -A written framework shall outline
A formal framework or policy outlining the hospital’s commitment, vision, goals, objectives and approach.
Ensure alignment with national regulations, accreditation standards, and the hospital’s strategic objectives.
3.1 Embed core Components of Clinical Governance
o Patient Safety: Implement incident reporting systems, safety walkarounds, and root cause analysis to proactively identify and address risks.
o Clinical Effectiveness: Apply evidence-based guidelines, care pathways, and standardized protocols to improve consistency and outcomes.
o Risk Management: Maintain risk registers, perform regular risk assessments, and implement mitigation strategies.
o Clinical Audit: Conduct scheduled audits with feedback loops and action plans to ensure accountability and improvement.
o Education and Training: Provide mandatory training, CME programs, simulation exercises, and thorough onboarding for new staff.
o Patient Involvement: Use surveys, patient councils, and feedback mechanisms to embed the patient voice in improvement plans.
o Staff Engagement: Foster a just culture, psychological safety, and leadership development to empower healthcare teams.
o Credentialing and Scope of Practice: Verify qualifications and ensure clinicians practice within approved roles and privileges.
o Policies and Protocols: Develop, review, and update clinical guidelines, policies, and procedures regularly.
o Annual Quality Improvement Plan: Establish and monitor a hospital-wide QI plan, setting priorities and measuring progress each year.
3.2 Establish reporting and escalation processes
3.3 Establish links to quality improvement and corporate governance
3.4 Create Performance Monitoring Systems
Define KPIs (Key Performance Indicators) for quality and safety (e.g., infection rates, readmission rates, patient experience scores).
Use dashboards and balanced scorecards to track progress and inform decision-making.
3.5 Review and Improve the Clinical Governance System
Conduct periodic self-assessments or external reviews.
Update the framework and processes based on lessons learned, changes in standards, or organizational growth.
4. Map Existing Activities
Review current safety and quality activities such as incident reporting, audits, morbidity and mortality reviews, and staff training.
Identify gaps and overlaps to prioritize areas for development.
5. Provide Training and Foster Culture
Deliver orientation and training programs to familiarize staff with clinical governance principles.
Promote a “just culture” that balances accountability with learning from errors.
Encourage open communication, respect for clinical leadership, and strong interdisciplinary collaboration.
6. Support a Culture of Continuous Improvement
Create safe systems for reporting, learning, and open dialogue on quality and safety.
Recognize excellence and empower teams to lead quality improvement (QI) initiatives.
Embed QI into staff performance appraisals, professional development, and career progression.
Running Clinical Governance Effectively: Sustaining the System
Regular meetings and reporting: Ensure the Clinical Governance Committee meets consistently and reports findings to senior management and the board.
Performance monitoring: Track key clinical indicators, safety events, and quality improvement outcomes.
Annual review: Evaluate the effectiveness of the governance system and adjust the structure or processes as needed.
Celebrate success: Recognize achievements and innovations that result from clinical governance efforts.